Antibiotics: Why You Feel Awful After Taking Them
By Dr. Shawn Bladel | July 8, 2025 | Recreated Health
Introduction
Antibiotics have been one of modern medicine’s greatest achievements. They’ve saved countless lives from infections that once proved fatal. When used at the right time and for the right condition, they remain incredibly valuable.
But here’s the part that often gets overlooked: antibiotics don’t come without a cost. Many patients report that after finishing a prescription, they feel drained, anxious, foggy, or just “off.” If that’s been your experience, you’re not alone.
At Recreated Health, I teach patients that antibiotics are a double-edged sword. They target harmful bacteria, but they also wipe out the beneficial microbes that keep your body resilient. The fallout can affect everything from digestion and mood to hormones and long-term immune health.
Let’s explore exactly why antibiotics can make you feel so awful, and—most importantly—what you can do to restore balance naturally.
The Gut Microbiome: Your Inner Ecosystem
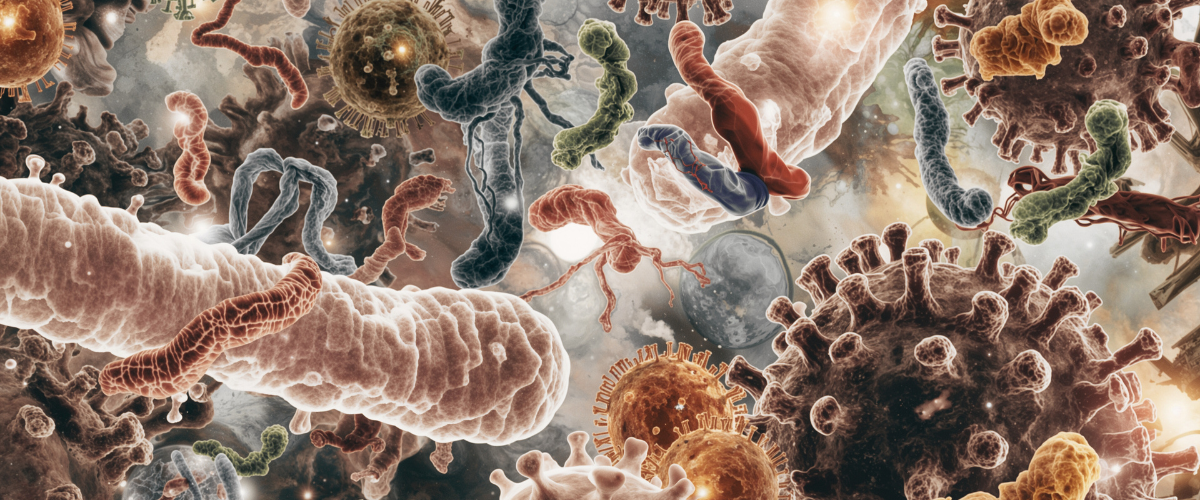
Your gut is home to trillions of microbes—bacteria, fungi, and even viruses—that form what we call the microbiome. This inner ecosystem is critical to nearly every part of your health.
Beneficial bacteria in your gut:
- Break down food and extract nutrients
- Produce vitamins like B12 and K2
- Regulate your immune system
- Help balance hormones
- Even manufacture neurotransmitters like serotonin and dopamine that affect your mood [3][4]
When you take antibiotics, they don’t discriminate. They kill both the harmful bacteria causing infection and the beneficial bacteria your body relies on every day [2][5]. The result is a gut ecosystem that becomes destabilized, opening the door to inflammation, mood changes, and chronic symptoms.
Why You Feel Awful After Antibiotics
1. Gut Dysbiosis: Loss of Good Bacteria
One of the most immediate consequences of antibiotics is gut dysbiosis—an imbalance between good and bad microbes. With beneficial bacteria wiped out, harmful bacteria and yeast (like Candida) can take over.
This imbalance often shows up as bloating, gas, constipation or diarrhea, and even new food sensitivities [5]. But the effects go deeper. Dysbiosis can impair nutrient absorption, weaken immune function, and set the stage for long-term digestive struggles.
👉 What helps: Replenishing the microbiome with a multi-strain probiotic and adding fermented foods such as sauerkraut or kefir to your diet.
2. Leaky Gut: Damage to the Gut Lining
The gut lining is like a protective filter. It allows nutrients to pass into your bloodstream while keeping toxins, pathogens, and undigested food particles out. Antibiotics can weaken this barrier, creating what’s known as leaky gut [6].
When the gut lining becomes permeable:
- Inflammation spreads throughout the body
- The immune system overreacts to everyday foods
- Toxins and microbes slip into the bloodstream, triggering more systemic problems
Symptoms of leaky gut can look like skin breakouts, weight changes, painful menstrual cycles, joint pain, and brain fog [7].
👉 What helps: Nutrients like L-glutamine, collagen, and zinc carnosine to repair the gut lining, paired with an anti-inflammatory diet free of processed sugars and seed oils.
3. Neurotransmitter Disruption: Mood & Brain Fog
Did you know that over 90% of serotonin—the “feel good” neurotransmitter—is made in the gut? When antibiotics disrupt beneficial bacteria, production of serotonin, dopamine, and GABA drops [8].
This explains why many people feel anxious, irritable, or depressed after a course of antibiotics. Brain fog and poor focus are also common because the gut-brain connection is disrupted.
👉 What helps: Gut-brain support through probiotics, adaptogens like ashwagandha, and calming minerals such as magnesium.
4. A Weakened Immune System
Ironically, while antibiotics are prescribed to fight infections, they can weaken your long-term defenses. That’s because 70–80% of your immune system lives in the gut [9]. When the gut microbiome is disrupted, immune balance suffers.
This can lead to recurring infections, poor recovery from illness, and even autoimmune flare-ups [10]. I often see this pattern in patients struggling with chronic Lyme, mold, or parasitic infections—the immune system is simply too drained to fight effectively.
👉 What helps: Supporting immunity with vitamin D, zinc, and immune-balancing probiotics.
5. Toxin Build-Up & Detox Pathway Stress
When bacteria are killed, they release endotoxins. If your liver and detox pathways are already overburdened, these toxins build up, causing headaches, fatigue, joint pain, and skin issues [11]. This “die-off” effect can feel like the flu.
👉 What helps: Staying hydrated with mineral-rich water, using gentle binders like BioToxin Binder, and supporting the liver with NAC, milk thistle, or glutathione precursors.
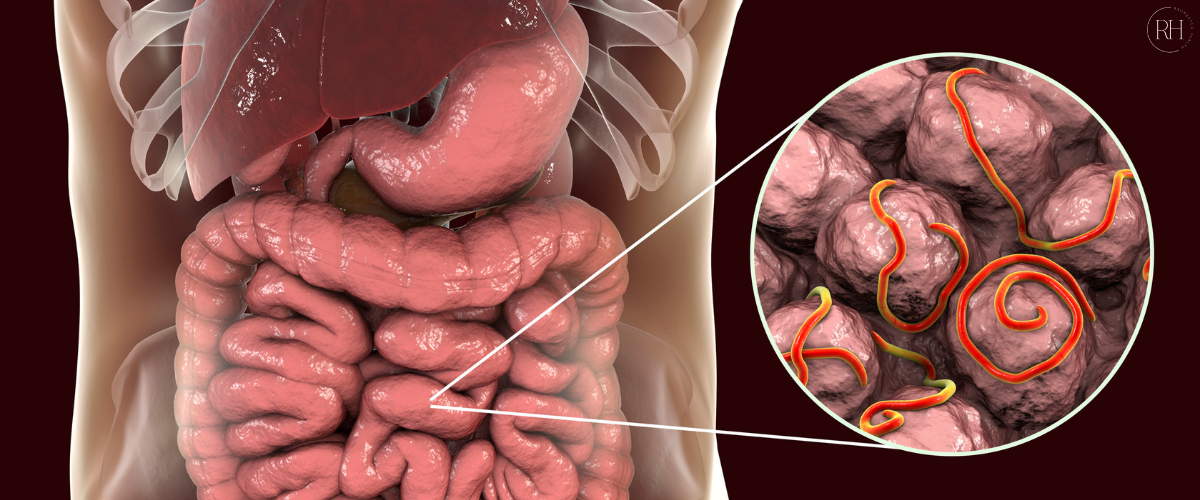
6. Opportunistic Infections: Candida & Parasites
Without healthy bacteria to guard the gut, opportunistic organisms often move in. Candida overgrowth is common, leading to sugar cravings, fatigue, and brain fog. Parasites can also take advantage of weakened defenses, adding more stress to the thyroid, liver, and immune system.
👉 What helps: Antifungal herbs, a guided parasite cleanse, and ongoing microbiome support.
The Antibiotic–Thyroid & Hormone Connection
Antibiotics don’t just affect digestion—they can disrupt hormones too.
- Leaky gut and dysbiosis fuel chronic inflammation, which can trigger autoimmune thyroid conditions like Hashimoto’s [12].
- A stressed gut and liver struggle to metabolize estrogen, leading to heavy cycles, PMS, and mood swings.
- The liver also plays a critical role in converting thyroid hormone (T4 into active T3). When stressed, this conversion slows, leaving you fatigued and sluggish [13].
This is why many patients experience lingering fatigue, stubborn weight, and hormonal symptoms long after their prescription ends.
Supporting Recovery After Antibiotics
If antibiotics are unavoidable, the key is to help your body bounce back quickly. Here’s the approach I use at Recreated Health:
1. Repopulate the Gut
- Take a multi-strain, practitioner-grade probiotic
- Eat fermented foods like kimchi, kefir, or sauerkraut
👉 [Shop Probiotic Support Here]
2. Repair the Gut Lining
- Supplement with L-glutamine, collagen, and zinc carnosine
- Eat an anti-inflammatory diet rich in whole, unprocessed foods
👉 [Explore Gut-Healing GI Revive]
3. Support Detox Pathways
- Drink mineral-rich filtered water
- Use gentle binders for toxin clearance
- Add liver support like NAC, milk thistle, or glutathione precursors
👉 [Detox Support Supplements]
4. Balance Mood & Hormones
- Use adaptogens (ashwagandha, rhodiola)
- Add magnesium glycinate and B vitamins for nervous system balance
- Consider seed cycling or gentle liver detox for female hormone support
5. Address Opportunistic Infections
- Complete a Candida or parasite cleanse under professional guidance
👉 Parasite Detox Blueprint eBook

Testing & Retesting
To truly understand your gut after antibiotics, I recommend starting with:
- Stool testing (GI-MAP, OAT test) → dysbiosis, parasites, yeast, gut markers
- Bloodwork → vitamin D, zinc, magnesium, B12
- Thyroid and Hormones panel → thyroid (TSH, Free T4, Free T3, antibodies) and complete sex hormones panel
📅 Retesting every 3–6 months ensures progress is measured and your plan evolves with your body.
Key Takeaways
- Antibiotics kill harmful and beneficial bacteria, creating gut imbalance.
- This imbalance can cause leaky gut, mood changes, hormonal issues, and autoimmune flares.
- Candida and parasites often flourish afterward.
- Supporting gut repair, detox, hormones, and immune function is critical to recovery.
Next Steps
Ready to recover your gut after antibiotics?
- 📘 Download my Parasite Detox Blueprint eBook → Shop Now
- 🌱 Explore Gut-Healing Supplements → Browse Here
- 💬 Schedule a Consultation with Dr. Shawn Bladel → Book Here
Your body has an incredible ability to heal when you give it the right support.
References
Liu X, et al. Gut-liver axis and thyroid hormone metabolism. Endocr Rev. 2018.
Blaser MJ. Antibiotics and the human microbiome. Nat Rev Microbiol. 2016.
Becattini S, et al. Impact of antibiotics on the gut microbiota. Nat Rev Microbiol. 2016.
Dinan TG, Cryan JF. Gut microbiota and mental health. Mol Psychiatry. 2017.
O’Mahony SM, et al. Microbiome-gut-brain axis and mood disorders. Neurogastroenterol Motil. 2015.
Francino MP. Antibiotics and alteration of the gut microbiota. Front Microbiol. 2016.
Mu Q, et al. The gut microbiome and autoimmunity. Clin Rev Allergy Immunol. 2017.
Fasano A. Leaky gut and autoimmune disease. Clin Rev Allergy Immunol. 2012.
Kelly JR, et al. Breaking down the gut-brain axis. Trends Neurosci. 2015.
Belkaid Y, Hand T. Role of the microbiota in immunity. Science. 2014.
Honda K, Littman DR. The microbiome in autoimmune disease. Nature. 2016.
Nicholson JK, et al. Host-gut microbial interactions and metabolism. Science. 2012.
Chistiakov DA. Gut microbiota and thyroid autoimmunity. World J Gastroenterol. 2014.